19 December 2017
The Case for Disinfectants - 6 Reasons Antibiotics are Not Your Best Friends
Viroxy analyses our options in managing healthcare associated infections and explains the reasons to practice proper infection prevention methods to limit antibiotics dependence.

In 2014, the National Institute for Health and Care Excellence, a government health agency in the UK reported 1 in every 16 patients treated at NHS hospitals acquire healthcare associated infections (HAIs). In the US, the Centres for Disease Control (CDC) estimated approximately 1.7 million HAI cases resulting in 99,000 deaths each year.
HAI occurs when patients seeking treatment at a healthcare facility acquire an infection unrelated to their original medical conditions due to compromised hygiene procedures. This could be attributed to poor hand hygiene practice among staff or inadequate disinfection/sterilisation of medical instruments and surfaces. Once an infection occurs, doctors have no choice but to turn to antibiotic treatment.
The age-old adage ‘prevention is better than cure’ has never been more relevant than now with antibiotics increasingly losing the battle against HAIs. To fully appreciate the necessity of prevention, we first need to understand the basics: the cell structure of a bacterium, how disinfectants work, how antibiotics work and the limitations of antibiotics.
Cell structure of a bacterium
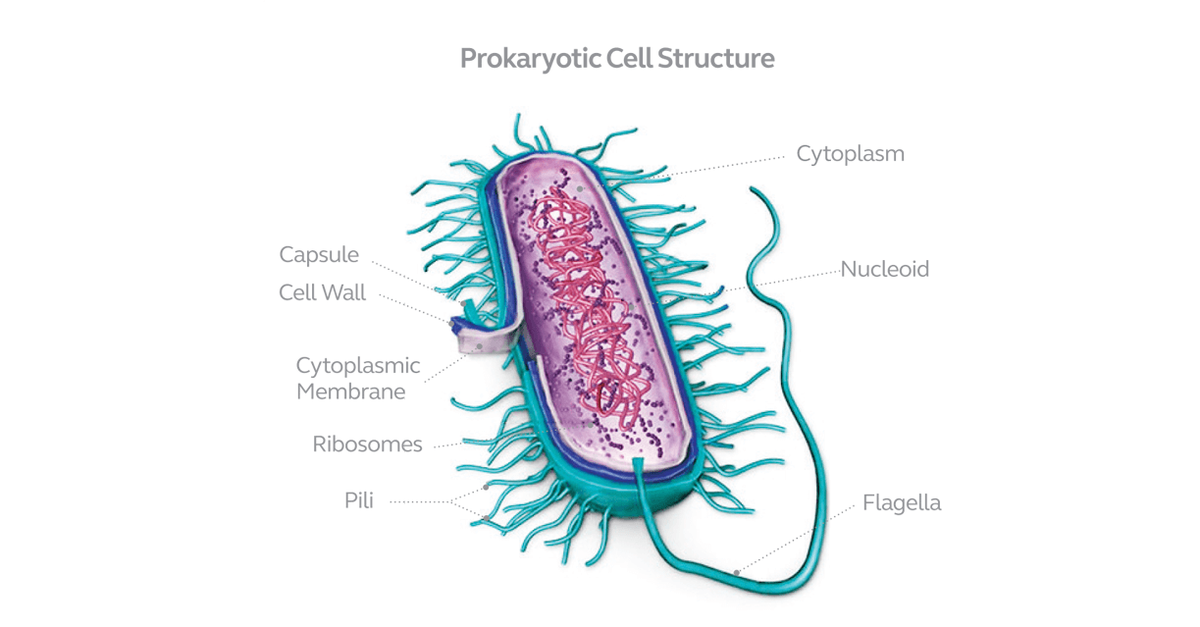
A typical bacterium is made up of cytoplasm where cell activities take place, nucleoid containing strands of DNA, ribosomes, pili to help the bacterium attach itself to other cells and surfaces, flagella to move, cytoplasmic membrane and cell wall.
The cell wall is composed of peptidoglycan, a polysaccharide molecule that envelopes the cytoplasmic membrane to help the cell maintain its shape. It also protects the cell from the environment such as changing osmotic pressure.
Cell wall composition varies among bacteria and it is one of the most important factors in bacterial species differentiation. And in the development of a destruction mechanism against the microorganism.
How disinfectants work
The active ingredients in a disinfectant determine the effectiveness of the product. Some commonly used ingredients are alcohol, quaternary ammonium compound, alkylamine and hydrogen peroxide. Although each active ingredient works against bacteria in its own way, the typical mechanism involves attacking lipid membranes to breakdown the structural integrity of the microorganism. This is followed by denaturing the protein in the bacterium to disrupt essential functions such as cell protection, energy generation, motion, surface attachment and DNA transfer which eventually leads to cell lysis. Although it seems complex, in real life, the process only takes between a few seconds to a few minutes depending on the active ingredient.
How antibiotics work
Alexander Fleming discovered the first antibiotic known as penicillin in 1928 when a rare strain of fungus excreted a substance that inhibited bacterial growth. Since then, many types of antibiotics have been discovered and used in the healthcare industry, leading to a new era of dependence, misuse and overuse of the drug.
Different classes of antibiotics work differently in killing bacteria. Beta-Lactam antibiotics for example, prevent bacteria from building cell walls causing the pressure in the cell to increase and eventually explode. Macrolides block bacterial ribosomes and prevent them from building life-crucial proteins. Quinolones break DNA strands and prevent them from being repaired which kills the bacteria.
Antibiotics are usually administered orally, intravenously or as suppositories depending on patient condition and suitability.
Limitations of antibiotics
Although both disinfectants and antibiotics achieve the same outcome in destroying bacteria, they work in wholly different settings. Disinfectants are used in the external environment while antibiotics work inside the body where the effects are hard to control. There are also other limitations to antibiotics when compared to disinfectants. Let’s analyse 6 of them:
- Antibiotics do not discriminate between the good and bad bacteria - Some bacteria that reside in our bodies naturally are essential to our wellbeing. Escherichia coli for example, can be found in large intestines to help the digestion process and vitamin K production. Only certain strains of E. coli are harmful to health. Another example is Bacteroides thetaiotaomicron which helps to break down plant molecules to aid digestion. A single course of antibiotics kills both the good and bad bacteria. This is less of an issue with disinfectants as they work outside the body.
- Bacteria build resistance over time - This happens when a course of antibiotics is not completed, leaving bacterial colonies to survive, mutate and build resistance against the drug. In recent years, more and more experts have cautioned doctors against prescribing antibiotics when it is not absolutely necessary. Earlier this year, the World Health Organisation (WHO) announced 12 antibiotic resistant bacteria that pose increasing threat to human lives and divided them into three categories to prioritise the urgency for new antibiotics. It may take several years for researchers to find replacement drugs for bacteria that are resistant to multiple antibiotics. In the meantime, these virulent bacteria continue to infect unsuspecting patients in hospitals and clinics with poor infection control, forcing them to go through long recovery processes, leaving others with weakened immune system to succumb.
- Antibiotics are only effective against bacteria - Antibiotics are not effective against fungi, viruses and other microorganisms that are pathogenic in nature. Each infection requires a different type of drug or medication. Disinfectants generally have a broader spectrum of efficacy against microorganisms.
- Antibiotics cause side effects in some people - Certain antibiotics such as penicillin and cephalosporin cause adverse effect in some people. Symptoms include skin rash, diarrhea, yeast infections and sores. In others, antibiotics can trigger severe anaphylactic or allergic reactions such as wheezing, dizziness, swelling of the face, lips and tongue and increased heart rate.
- Complete recovery takes time - Antibiotics typically need a week of treatment before recovery. In cases involving antibiotic-resistant bacterial infections, it can take months or even years of treatment. This does not include the time required to re-cultivate the good bacteria destroyed during antibiotic treatment.
- Costly - Although this is not specific to antibiotics, relying on treatments instead of prevention is a costly affair in general. This is even more so in HAI cases where patients require treatment for a condition they did not have in the first place. The economic burden this entails through hospitalisation, medication, absence from work and other indirect costs can be damaging in the long run. In the US, CDC reported $20 billion in healthcare costs due to HAIs every year.
These 6 points make a good case for disinfectants and prevention as opposed to antibiotics and treatment. It is so much easier, safer, faster and cheaper to practice good infection control methods from the outset and keep infectious diseases under control.
Are you going the extra mile in our battle against antibiotic-resistant infections? How many antibiotic-resistant microorganisms is your product effective against?
Call us at +60 (0)3 2630 8888 to test your disinfectant against antibiotic resistant microorganisms.
Download PDF file
